The Citizens Commission on Human Rights filed Freedom of Information Act requests across 32 states to obtain data on psychiatric drug prescribing to children enrolled in Medicaid. They shared that data with me for review. What it contains should prompt serious national conversation.
Medicaid is a federal and state program funded by American taxpayers, designed as a safety net for the country’s most economically vulnerable citizens. In 32 states alone, that safety net spent $1.78 billion prescribing psychiatric “medications” to nearly three million children in a single year. 270,000 of those children were under the age of five.
These are not benign interventions. They are drugs with serious, documented risks prescribed to developing brains during the most sensitive years of human life. Stimulants carry the same DEA addiction classification as OxyContin and fentanyl. Antidepressants carry a black box warning for suicidal behavior in children and adolescents and are associated with permanent neurological and sexual damage that may persist long after the drug is stopped. “Anti-anxiety” drugs including benzodiazepines carry warnings for life-threatening dependence in adults taking them for more than two weeks.
We are giving them to toddlers.
Not one of these drug classes carries FDA approval for children under five. Every one of them is being prescribed to children under five, at scale, with taxpayer dollars.
Medical ethics and medical law both require informed consent, the protection of vulnerable populations, and the subordination of financial incentive to patient welfare. What this data describes is a systematic departure from all three. The ethical failure is visible in every prescription written without a conversation about risk. The legal exposure is written into every Medicaid claim where informed consent was never adequately obtained.
This is what it looks like from inside one appointment.
A mother brings her six-year-old to the pediatrician. He’s been disruptive at school. Can’t sit still. Talks back. Cries too easily. The appointment lasts eight minutes.
She leaves with a prescription.
Nobody asked whether he’d witnessed violence at home. Nobody asked if he was sleeping in the same bed as three siblings, or going to school hungry, or living with a parent who drank too much, or grieving a father who left, or had simply never had one consistent adult in his life who made him feel safe. Nobody asked if he was a six-year-old boy doing exactly what six-year-old boys do when their world is unstable and nobody has taught them what to do with the feeling.
This is who is on Medicaid. Single mothers working two jobs. Foster children cycling through placements. Kids in rural counties where the nearest psychiatrist is two hours away. Families who immigrated and don’t speak the language well enough to push back. People who trusted a doctor because they had no reason not to and no resources to seek a second opinion. These are not patients with too many choices. These are families with almost none.
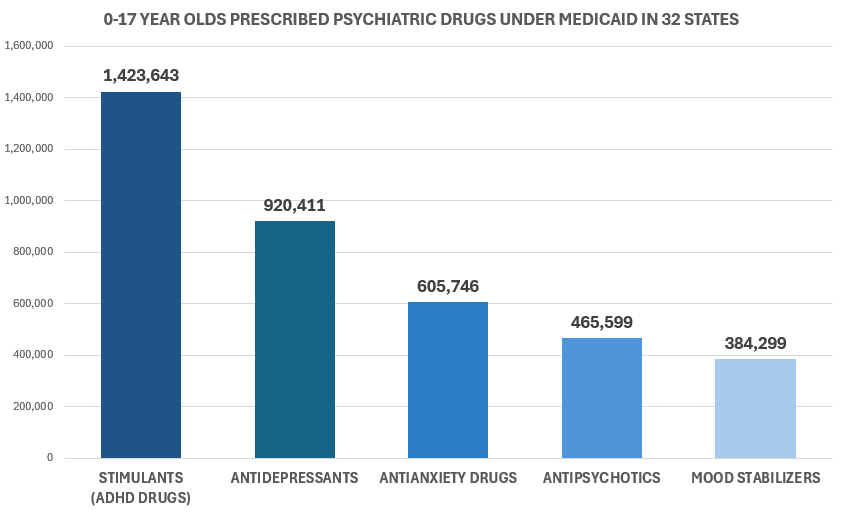
The following charts represent Medicaid psychiatric drug prescribing data obtained from 32 states in 2023. Every bar is a drug class. Every number is a child.
The data spans 32 states. Several findings stand out immediately.
New Jersey alone prescribed psychiatric drugs to over 400,000 Medicaid-enrolled children. Texas, with 2022 data, reported nearly 282,000. These are not small numbers buried in a large dataset. They are individual children in individual appointments who left with a prescription.
Oregon is the most striking outlier. A state with a total Medicaid enrollment of just over 700,000 children prescribed psychiatric drugs to 37.7% of them. More than one in three children on Oregon Medicaid received a psychiatric drug in a single year. And the top drug class in Oregon is not stimulants. It is antipsychotics. Drugs linked to permanent involuntary movement disorders, sudden death, and significant metabolic disruption including weight gain, insulin resistance, and type 2 diabetes. We are giving children drugs that damage their brains and their metabolic health simultaneously, then will likely treat the resulting obesity and diabetes as separate medical problems, with separate drugs, billed separately to Medicaid.
These are not anomalies I am selecting to make a point. They are what the data surfaces when you read it carefully.
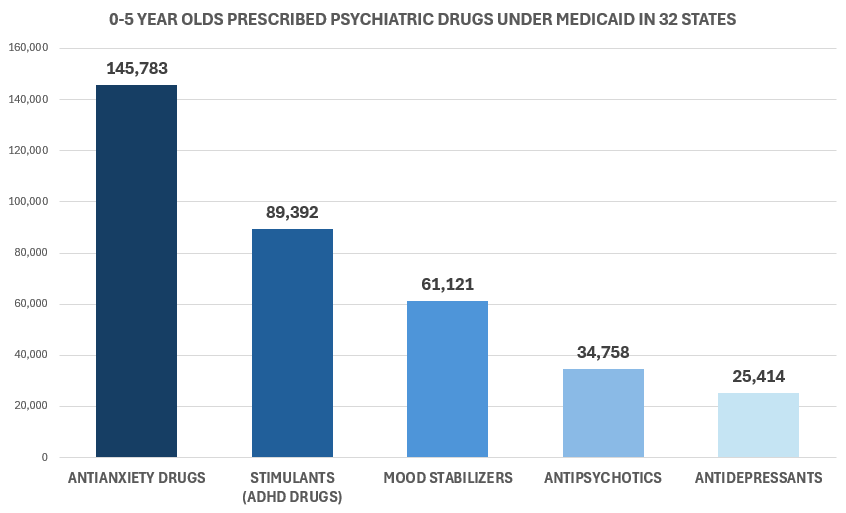
Now look at the children under five.
Nationally across the 32 states, the most prescribed drug class for children under five is not stimulants. It is anti-anxiety drugs, including benzodiazepines. Drugs so dependency-forming that adult patients are warned not to take them for more than two weeks. In Oregon, the top drug class for toddlers and infants is antipsychotics. In New Jersey it is mood stabilizers. In Texas, Florida, North Carolina, Georgia, California, Tennessee, New York, Kentucky, Illinois, Michigan, Oklahoma, and Pennsylvania, the top prescribed class for children under five is anti-anxiety medication.
This is happening in nearly every state that reported. It is not an outlier. It is the pattern. These are not the full numbers. They are what 32 states reported. The 18 states not represented include some of the most populous in the country.
The prescribing data tells us how many children are on these drugs. It does not tell us who is prescribing them, at what volume, or what financial incentives are driving the decisions. A separate and more granular disclosure, also obtained by the Citizens Commission on Human Rights, begins to answer those questions.
But before we get to individual prescribers, consider what this scale requires of any clinician. Genuine psychiatric care for a child demands time. It demands a thorough understanding of that child’s life, home environment, developmental history, sleep, nutrition, and the conditions that are actually driving their distress. It demands a conversation with parents or caregivers that covers risks, alternatives, and what the FDA’s own warnings say about these drugs in children.
That cannot be done in a brief appointment. It cannot be done at high volume. And at the scale this data describes, across millions of children, it is not being done at all. What is happening instead is not evaluation. It is processing. Children moving through a system that has no financial incentive to slow down and every financial incentive to keep the line moving.
Illinois is currently the only state where prescriber-level Medicaid data has been made available. That distinction matters. Aggregate numbers reveal the scale of the problem. Prescriber-level data reveals the mechanism. It shows exactly how a system built around financial incentives operates when nobody is watching. The question it raises is not just what is happening in Illinois. It is why every state in the country does not make this data publicly available as a matter of course. The fact that it doesn’t is itself part of the answer.
The top prescriber in Illinois is a clinical nurse specialist, not a psychiatrist. In a single year she prescribed psychiatric drugs to nearly 4,000 Medicaid-enrolled children across every drug class: stimulants, antidepressants, antipsychotics, mood stabilizers, and anti-anxiety drugs. She has held the position of top prescriber in the state for six consecutive years. Her Medicaid reimbursement for ADHD drugs alone was $203,711 in one year. That figure does not include reimbursement for the other drug classes she prescribed to hundreds of additional children.
Consider what 4,000 children in one year actually requires. It means evaluating, diagnosing, and prescribing to more than 15 children every working day. There is no model of genuine clinical care that supports that volume.
The financial architecture of the system makes this not just possible but predictable. A Medicaid psychiatric medication management appointment generates reimbursement whether it lasts twelve minutes or sixty. A prescription generates drug reimbursement on top of that.
Illinois has enacted a school mental health screening mandate that generates a pipeline of referrals feeding directly into that billing structure. Children are screened. Screenings produce diagnoses. Diagnoses produce prescriptions. Prescriptions produce revenue. Every step is funded by tax dollars. None of it requires that the child actually gets better.
The names of the top prescribers in Illinois are being withheld here. Active regulatory complaints have been filed against several of them and those proceedings are ongoing. What cannot be withheld, because it is documented in public Medicaid data, is the pattern. A small number of providers, operating at volumes no legitimate clinical practice could justify, are generating substantial Medicaid revenue from the poorest and most vulnerable children in the state. Year after year. Without investigation. Without interruption. Without consequence.
There is no reason to believe Illinois is unique. It is simply the state where someone looked.
The CCHR data captures prescriptions. It does not capture consequences. What happens to a child after that prescription is filled is not tracked, not reported, and not the concern of any federal agency with the authority to act on it.
The regulatory failures that allowed this prescribing culture to take root, including the documented suppression of evidence showing antidepressants increase suicidal behavior in children, fail to outperform placebo in pediatric populations, and carry risks that regulators chose to bury rather than disclose, are covered in depth here:
The Big Lie: How Antidepressants for Teens Became "Evidence-Based Medicine"
The permanent neurological and sexual damage now documented in patients who took these drugs, including teenagers who will spend years or decades living with consequences they were never warned about, is covered here:
How Antidepressants Are Numbing More Than Depression
Both of those pieces are part of the same story. This is the data that makes the scale of that story visible.
Let’s be clear about what these drugs do to children in the short term. They sedate. They blunt. They make a dysregulated, distressed, or frightened child easier to manage. For school-age children that might mean a classroom. For the 270,000 children under five in this data, we are not talking about classrooms. We are talking about homes, daycares, and foster placements. Infants and toddlers whose distress, whose crying, whose inability to be soothed, are being chemically suppressed before they can speak, before they can walk, before they have any capacity whatsoever to communicate what is happening to them or to refuse what is being given to them.
Among these youngest children are some of the most vulnerable human beings in the country. Children born to mothers who struggled with addiction during pregnancy. Children born into poverty and instability who entered Medicaid at birth and encountered a system with no tools beyond a prescription pad. Children of parents with psychiatric diagnoses of their own.
There is no scientific evidence that prescribing psychiatric drugs to infants and toddlers prevents the development of psychiatric illness. None. These children are not being treated ethically or safely.
The Citizens Commission on Human Rights has outlined immediate policy demands that represent the minimum structural response to what this data reveals. They are necessary. They are not sufficient. But they are where accountability must begin.
Immediate Policy Requirements
1. Mandate FDA Medication Guide distribution as a condition of Medicaid reimbursement. Every parent or guardian must receive a printed FDA Medication Guide in plain language before any psychiatric drug is prescribed to their child. Signed acknowledgment must be retained in the patient record. Prescriptions issued without documented compliance are ineligible for Medicaid reimbursement. Providers who repeatedly violate this requirement are barred from prescribing psychiatric medications under Medicaid.
2. Require CMS to identify and investigate high-volume prescribers. State Medicaid agencies must submit quarterly reports on the highest prescribers of psychiatric drugs to children. Providers prescribing to children under five, where virtually all such prescriptions are off-label and lack FDA approval for that age group, must be subject to immediate audit. Medicaid funds must stop flowing to providers whose prescribing patterns no legitimate clinical practice could justify.
3. Establish an independent, conflict-free expert panel to review psychiatric drug risks. The FDA possesses years of clinical trial data, post-marketing reports, and adverse event findings that have never been independently reviewed by researchers without pharmaceutical ties. A standing panel reporting directly to the Secretary of Health and Human Services and to Congress, with no industry funding and binding authority, must be established to evaluate what that data actually shows.
4. Build a federal adverse drug reaction database under CMS. There is currently no systematic mechanism for tracking what happens to Medicaid-enrolled children after psychiatric drugs are prescribed. A mandatory, streamlined, publicly accessible adverse drug reaction reporting system must be created, with financial penalties for Medicaid agencies that fail to comply. Without it we are operating without the most basic feedback loop medicine requires.
These measures address the immediate failures of oversight, consent, and accountability. They do not address the foundational question this data forces us to confront.
How did we allow this to happen?
Not through malice, in most cases. Through a series of choices, each one made within a system that rewarded a certain kind of answer and penalized the harder ones. Physicians trained inside a pharmacological model who genuinely believed they were helping. Researchers whose funding depended on findings that supported prescribing. Regulators whose budgets depended on the industry they were meant to oversee. Legislators who received campaign contributions from the pharmaceutical industry and trusted the experts that industry paid to testify. Parents who trusted the doctors. Caregivers in impossible circumstances who had a child in front of them they did not know how to help and a system offering them one solution.
We built institutions that were supposed to protect the most vulnerable among us. We funded them with public money and public trust. And somewhere along the way, the protection became the harm, and the trust became the mechanism through which the harm was delivered.
These are children. The youngest, the poorest, the least protected. They arrived in this world already behind, placed into systems that were never built to truly care for them, and handed drugs by people who either did not know the risks or did not stop to ask. The decisions were made above them. The consequences live inside them.
They deserved better. They still do.
Children are not complicated. What they need is not a mystery.
They need safety. A home where they are not afraid. Adults who are present, consistent, and attuned to them. Enough food. Enough sleep. Enough time outdoors and in their bodies. Schools that understand them. Communities that include them. The experience, repeated enough times to become belief, that they matter and that the world is navigable.
When a child is struggling, the first question should be the simplest one. What is happening in this child’s life? What are they carrying that no child should have to carry alone? What do they need that they are not getting? Those questions take time. They require genuine attention, genuine relationship, and genuine care. They cannot be answered in twelve minutes. They cannot be answered with a prescription.
They can be answered. That is the point. The problems driving childhood distress are real and they are solvable, not with drugs, but with the kind of sustained, compassionate, human attention that we have systematically defunded in favor of a pharmacological shortcut.
We are paying for this system. Every American taxpayer is funding what this data describes. That means every American taxpayer has a legitimate claim on what this system does and does not do in their name. We have a right to demand that public money spent on the healthcare of vulnerable children is spent on care that is safe. Care that addresses actual problems.
We have a right to demand medicine that sees a suffering child and asks why before it asks what to prescribe. That treats the root before suppressing the symptom. That operates from the understanding that a child in distress is communicating something real about their life, and that the response that honors their humanity is not sedation but attention.
This is not idealism. It is the oldest and most basic standard of care. It is what we owe every child in this country, most especially the ones who have no one else advocating for them.
They deserve safety. They deserve compassion. They deserve time. They deserve adults and institutions that take their problems seriously enough to understand it. They deserve a system built around their healing rather than around the management of their symptoms for the comfort of everyone else.
That is the standard. We are nowhere near it. And the distance between where we are and where we need to be is not a reason for despair. It is a reason to act.
AWAKEN
Thank You!
Radically Genuine is a reader supported publication. No advertisers. No sponsors. No institutional funding. Your paid subscriptions make this work possible and allow me to continue dedicating time to what matters. More than that, we are building something here. A community of people who sense the shift and refuse to stay asleep. Thank you for being part of it.
Thanks for reading Radically Genuine ! This post is public so feel free to share it.